Answer of July 2016
For completion of the online quiz, please visit the HKAM iCMECPD website: http://www.icmecpd.hk/
Clinical History:
53 year old male sustained knee injury a year ago and complained of persistent knee pain.
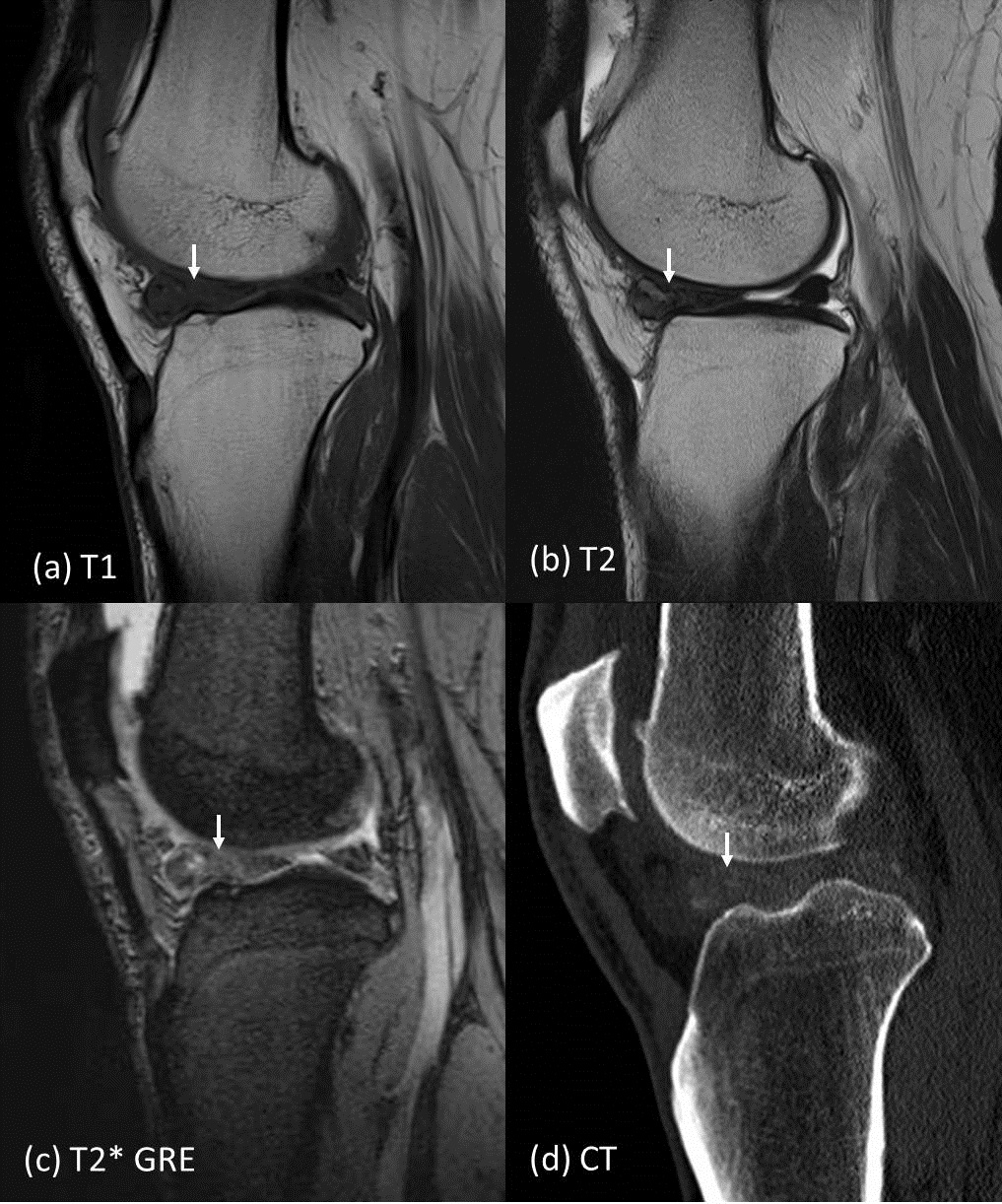
Figure 1
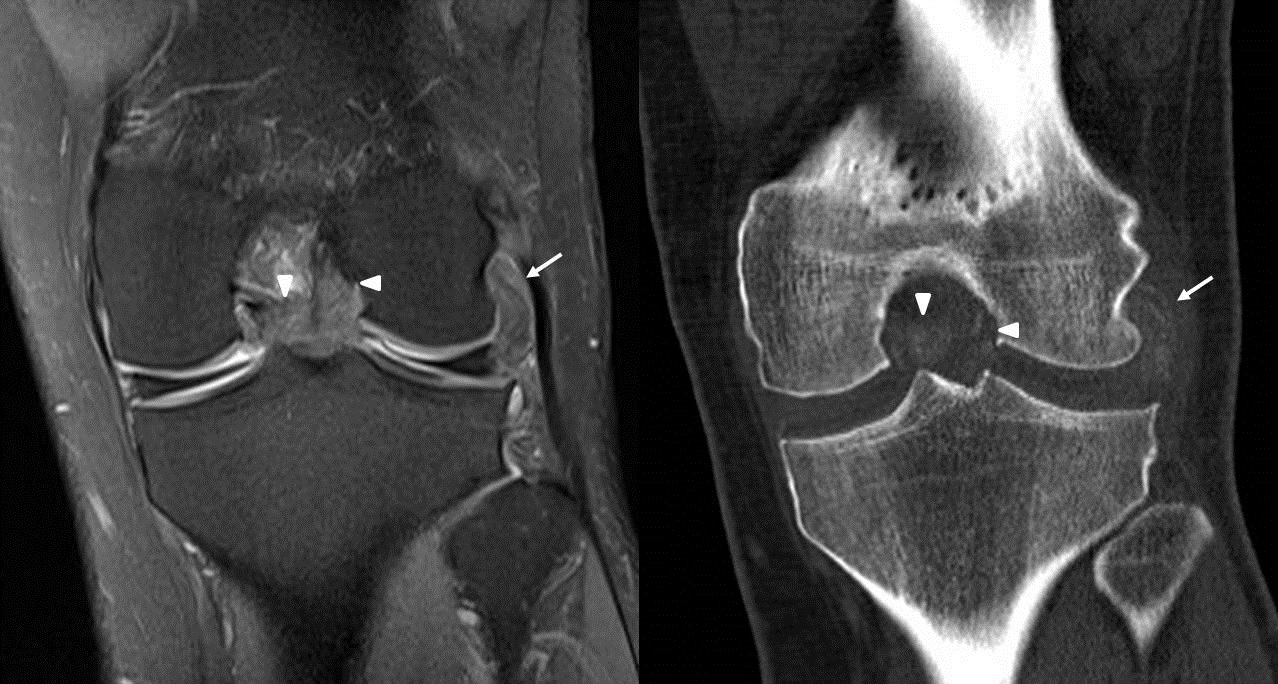
Figure 2
Diagnosis:
Intrameniscal gout
Discussion:
Plain MRI of left knee performed showing apparently enlarged anterior horn of lateral meniscus, with meniscal tissue being replaced by lobulated T1 intermediate T2 hypointense lesion (Fig. 1a,b). Lesion of similar signal intensity also noted infiltrating popliteus tendon (Fig 2 arrow), in intercondylar region around anterior and posterior cruciate ligaments (Fig 2 arrowhead). No blooming artefact is demonstrated by the lesion on T2* weighted gradient echo sequence (GRE) (Fig 1c). Supplementary CT was performed, showing calcification over the above mentioned regions (Fig 1d, 2). No bony erosion seen. Features are more suggestive of gouty tophi. In our patient, there is intrameniscal and intraligamentous gouty tophi. Serum urate level was shown to be high in subsequent blood test. Patient however has not previous history of gouty attack.
The MRI features of gout are variable, and it is well known to be a great mimicker. Intraarticular gout may even lead to misdiagnosis of intraarticular tumour. Tophi typically have intermediate or low signal intensity on T1-weighted images and heterogeneous signal intensity on T2-weighted or fluid-sensitive sequences, possibly because of the presence of variable amounts of calcium. Tophi can show uniform enhancement or show a nonenhancing center. Because of the somewhat nonspecific features of gout on MRI, clues to the correct diagnosis are site of involvement and distribution of findings. A common site of gout involvement is the knee. Specific tendons being affected in the knee is popliteus and patellar tendons. Intraarticular gouty tophi is not common, if present, usually in intercondylar notch, suprapatellar bursa, lateral gutter, tibial plateau. Intrameniscal gouty tophi is even rarer, with only two cases being described. In both cases, the tophi are arising from the lateral meniscus and the patients also did not recall any history of gouty attack, as in our case. There have been several reports regarding the treatment of intraarticular gout, which include medical treatment with allopurinol, or arthroscopic surgery.
A major differential diagnosis in this case would be pigmented villonodular synovitis (PVNS), especially the focal subtype, which is also T1 and T2 hypointense, and can present as intraarticular mass. One characteristic feature of PVNS would be the presence of blooming artefact, meaning augmented signal void on T2* weighted gradient echo sequence due to presence of hemosiderin deposits. Blooming artefact is absent in our patient. Calcification on CT is also supporting evidence for gouty tophus, but not for PVNS.